Table of Content
The following describes the steps in determining the annual estimated aggregate expenditures including the exclusions and assumptions made when simulating 60-day episodes from actual 30-day periods. For home health periods of care beginning on or after January 1, 2020, Medicare makes payment under the HH PPS on the basis of a national, standardized 30-day period payment rate that is adjusted for case-mix and area wage differences in accordance with section of the BBA of 2018. The national, standardized 30-day period payment rate includes payment for the six home health disciplines (skilled nursing, home health aide, physical therapy, speech-language pathology, occupational therapy, and medical social services). Payment for non-routine supplies is also part of the national, standardized 30-day period rate. Durable medical equipment provided as a home health service, as defined in section 1861 of the Act, is paid the fee schedule amount or is paid through the competitive bidding program and such payment is not included in the national, standardized 30-day period payment amount.
While Medicare systems may allow an edit to be bypassable , it does not currently allow an unacceptable home health principal diagnosis to be bypassable. Evaluate what the CY 2020 base payment rate should have been based on actual behavior changes and actual utilization. If two 30-day periods of care from the same provider reference the same OASIS assessment date , then we assume those two 30-day periods of care would have been billed as a 60-day episode of care under the 153-group system. This behavior assumption assumes that HHAs will change their documentation and coding practices and put the highest paying diagnosis code as the principal diagnosis code in order to have a 30-day period be placed into a higher-paying clinical group. The 2021 home health payment rule, as finalized by CMS, came out during a critical stretch in the public health emergency, shortly before another devastating wave emerged.
G. Request for Information: Health Equity in the HH QRP
Our clinical advisors reviewed the ICD-10-CM diagnosis code J18.2 which is currently assigned to the comorbidity subgroup respiratory 4 . However, respiratory 2 contains other pneumonia with unspecified organism (for example, J18.1 and J18.8). Clinically, J18.2 is similar to the other pneumonias in respiratory 2 and therefore, should be reassigned from comorbidity subgroup respiratory 4 to comorbidity subgroup respiratory 2. In addition, we evaluated resource consumption related to the comorbidity subgroups respiratory 2 and respiratory 4, and J18.2 and found no significant variations negating a reassignment. We identified 12 ICD-10-CM diagnosis codes related to crushing injury of the face, skull, and head that warrant reassignment. Through a phase-in approach may require larger temporary and permanent adjustments in the future.
Section 1895 of the Act allows for the provision of an addition or adjustment to the home health payment amount otherwise made in the case of outliers because of unusual variations in the type or amount of medically necessary care. Under the HH PPS and the previous unit of payment (that is, 60-day episodes), outlier payments were made for 60-day episodes whose estimated costs exceed a threshold amount for each HHRG. The episode's estimated cost was established as the sum of the national wage-adjusted per visit payment amounts delivered during the episode. The outlier threshold for each case-mix group or PEP adjustment defined as the 60-day episode payment or PEP adjustment for that group plus a fixed-dollar loss amount. For the purposes of the HH PPS, the FDL amount is calculated by multiplying the home health FDL ratio by a case's wage-adjusted national, standardized 60-day episode payment rate, which yields an FDL dollar amount for the case.
Resumption of Care
A RAP is not required for LUPA periods of care; however, it is more challenging to predict when a period of care will result in a LUPA since it’s based on variable thresholds. You can’t miss out on the possibility where the first 30-day care plan with the additional visits might produce better outcomes and the second 30-day period may not be needed and a LUPA can be avoided. Moreover, the risk LUPA can cause within the second 30-day period is easily tracked with the help of past data of your organization. This analysis will provide into which 30-day periods and what types of episodes would fall into LUPA categories in a PDGM environment. When you talk about LUPA, It is one of the contractual adjustments that currently make up the Medicare-certified home health prospective payment system.
Commenters believed that payment should not be tied to measure performance until a measure is thoroughly tested, evaluated, and has NQF-endorsement. They believe that measure methodology and implementation of individual measures should be sufficiently vetted prior to inclusion, and specifically part of the HH QRP prior to advancing to the expanded HHVBP Model. Commenters suggested that prior to adding new measures to value-based purchasing initiatives, measures should first be included in its related quality reporting program. After consideration of the public comments received, we are finalizing our proposals without modification. Measures; and the impact of the domains and quality measure concepts on organizational culture change.
Table F1—U.S. Bureau of Labor Statistics' May 2020 National Occupational Employment and Wage Estimates
Therefore, we proposed to reassign the ICD-10-CM diagnosis codes listed in Table 9 from clinical group E and clinical group A (MMTA-Other) to clinical group C . The following section proposed reassignment of 320 diagnosis codes to a different clinical group when listed as a principal diagnosis, reassignment of 37 diagnosis codes to a different comorbidity subgroup when listed as a secondary diagnosis, and the establishment of a new comorbidity subgroup for certain neurological conditions and disorders. Due to the amount of diagnosis codes proposed for reassignment this year, we posted the “CY 2023 Proposed Reassignment of ICD-10-CM Diagnosis Codes for HH PDGM Clinical Groups and Comorbidity Subgroups” supplemental file on the Home Health Prospective Payment System Regulations and Notices web page. The term itself stands for “Low Utilization Payment Adjustment,” which is a standard per-visit payment for episodes of care with a low number of visits.
In response to interested parties' questions regarding upper respiratory malignant neoplasms, we reviewed 14 ICD-10-CM diagnosis codes related to malignant neoplasms of the upper respiratory tract currently assigned to the comorbidity subgroup neoplasm 6 . We also determined that B78.9 strongyloidiasis, unspecified was assigned to clinical group C , and should be reassigned to clinical group K (MMTA—Infectious Disease, Neoplasms, and Blood-Forming Diseases) because it would be consistent with the assignment of the other strongyloidiasis codes. We also identified that N83.201 unspecified ovarian cyst, right side was assigned to clinical group A (MMTA—Other) and should be reassigned to clinical group J (MMTA—Gastrointestinal Tract and Genitourinary System) because it would be consistent with the assignment of other ovarian cyst codes. We proposed to reassign these two ICD-10-CM diagnosis codes' clinical groups as shown in Table 6.
Accordingly, we proposed to change the HHA baseline year for HHAs certified prior to January 1, 2019 and for HHAs certified during January 1, 2019-December 31, 2021 for all applicable measures used in the expanded Model, from CY 2019 and 2021 respectively, to CY 2022 beginning with the CY 2023 performance year. Additionally, we proposed that for any new HHA certified on or after January 1, 2022, the HHA baseline year is the first full calendar year of services beginning after the date of Medicare certification and the first performance year is the first full calendar year following the HHA baseline year. As such, we did not calculate or propose the CY 2023 wage index as if the cap was in place for 2022. While such a policy may benefit some providers, it would change the wage index budget neutrality factor, and would impact the CY 2023 payment rates for all providers without allowing them the opportunity to comment.
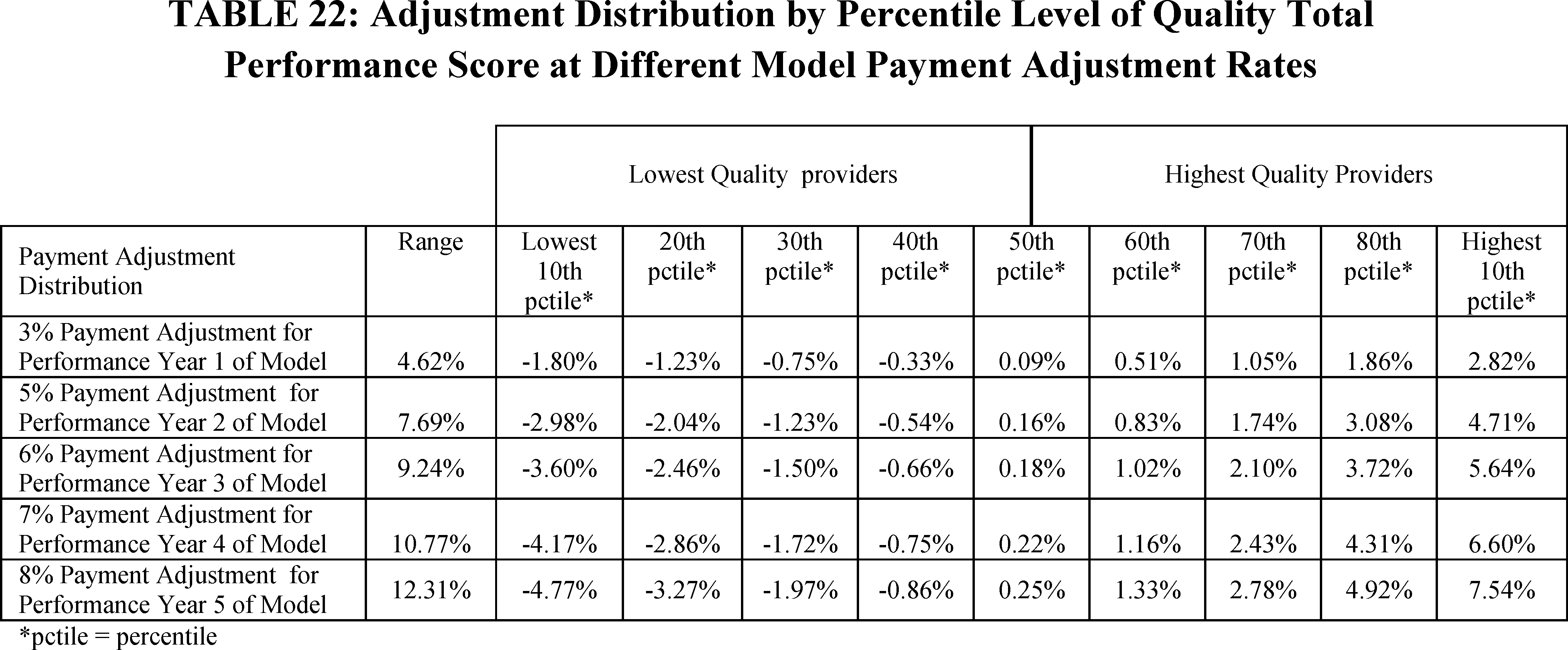
As shown in Table 3, an additional permanent prospective adjustment of −1.42 percent (assuming the −6.52 percent adjustment was already taken) would be required to offset for such increases in estimated aggregate expenditures in future years. Additionally, we determined that our initial estimate of the base payment rates required to achieve budget neutrality resulted in excess expenditures of approximately $1.2 billion in CY 2021. This would require a temporary adjustment factor to offset for such increases in estimated aggregate expenditures for CY 2021.
This final rule would not impose a mandate that will result in the expenditure by State, local, and Tribal Governments, in the aggregate, or by the private sector, of more than $165 million in any one year. We discuss the alternative we considered to the finalized change to the HHA baseline year for each applicable measure in the expanded HHVBP Model in section IV.B.2.b. Section 1895 of the Act authorizes the HH QRP, which requires HHAs to submit data in accordance with the requirements specified by CMS. Failure to submit data required under section 1895 of the Act with respect to a program year will result in the reduction of the annual home health market basket percentage increase otherwise applicable to an HHA for the corresponding calendar year by 2 percentage points. To neoplasm 1 in alignment with clinically similar diagnosis codes already assigned (for example, C11.0 malignant neoplasm of superior wall of nasopharynx). In addition, we evaluated resource consumption related to the comorbidity subgroup, neoplasm 1, as well as diagnosis codes, C30.0, C30.1, C31.0, C31.1, C31.2, C31.3, C31.8, C31.9, C32.0, C32.1, or C32.2 and found no significant variations negating a reassignment.

Of this rule, we proposed to replace the term baseline yearwith the terms Model baseline yearand HHA baseline yearto differentiate between two types of baseline years used in the expanded HHVBP Model. In addition, we stated in the CY 2023 HH PPS proposed rule that we were considering the adoption of a structural composite measure for the HH QRP, which could include organizational activities to address access to and quality of home health care for underserved populations. The composite structural measure concept could include HHA reported data on HHA activities to address underserved populations' access to home health care. An HHA could receive a point for each domain where data are submitted to a CMS portal, regardless of the action in that domain. In light of these considerations, we proposed a permanent approach that increases the predictability of home health payments for providers and mitigates instability and significant negative impacts to providers resulting from changes to the wage index by smoothing year-to-year changes in providers' wage indexes.
Commenters raised the need to address issues such as expanding gender categorizations and updating race categories for some groupings. Proposed rule and before the publication of the final rule , we would use such data, if appropriate, to determine the home health payment update percentage for CY 2023 in the final rule. • Claims where the claim occurrence code 50 date occurred on or after October 31 of that year. This exclusion was applied to ensure the simulated 60-day episodes contained both 30-day periods from the same year and would not overlap into the following year . This is done because any 30-day periods with an OASIS assessment date in November or December might be part of a simulated 60-day episode that would continue into the following year and where payment would have been made based on the “through” date.

A commenter requested that CMS propose an inflation adjustment to enable best practices and allow agencies to continue to provide a high level of care. Commenters stated that the low reimbursement rates would be detrimental to patient care and may cause HHA closures. The final LUPA thresholds for the CY 2023 PDGM payment groups with the corresponding Health Insurance Prospective Payment System codes and the case-mix weights are listed in Table B26.
After reviewing the CY 2021 home health claims utilization data we determined that visit patterns have stabilized. We believe that CY 2021 data will be more indicative of visit patterns in CY 2023 rather than continuing to use the LUPA thresholds derived from the CY 2018 data pre-PDGM. Therefore, we proposed to update the LUPA thresholds for CY 2023 using data from CY 2021. We reviewed Q82.0 for clinical group reassignment, as described in section II.B.3.4. During this review, we discovered Q82.0 is not currently assigned to a comorbidity subgroup when listed as a secondary diagnosis.
No comments:
Post a Comment